Printed from acutecaretesting.org
October 2013
Age-adjustment of the D-dimer cut-off value to improve the exclusion of thromboembolic events in older patients
INTRODUCTION
Acute pulmonary embolism (PE) is one of the leading differential diagnoses of acute chest pain and/or acute dyspnea in the emergency department. Along with clinical risk stratification by the Geneva or Wells Score, respectively, testing the fibrin degradation product D-dimer is a key element in the point-of-care diagnosis of an acute PE and deep vein thrombosis (DVT) [1].
The combination a low clinical probability with a D-dimer blood test under the test-specific cut-off value (<0.5 mg/L in most assays) can safely rule out a thromboembolic event [2,3].
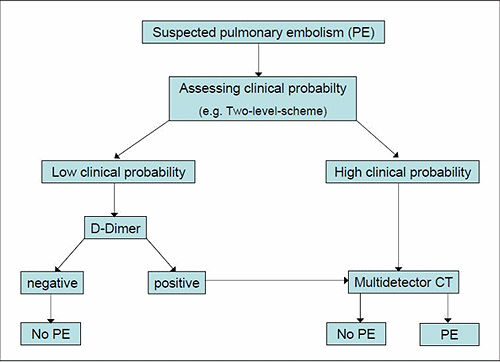
FIG. 1: Simplified diagnostic algorithm for patients with suspected venous thromboembolism, according to the European Society of Cardiology [1]. The Clinical probability assessed according to e.g. Wells Score [21].
EFFECTS OF AGE ON THE D-DIMER TEST
In elderly patients, the incidence of venous thromboembolism and its complication steadily increases [4]. In contrast, however, the diagnostic accuracy of the D-dimer test excluding a thromboembolic event decreases in these age groups.
Due to various mechanisms such as higher fibrinogen concentration, reduced renal elimination, (occult) malignant diseases and chronic inflammatory processes, an unspecific increase of D-dimer in blood is observed in elderly patients [5].
As a result, the specificity of the D-dimer test to rule out an acute PE/DVT declines in elderly patients, leading in turn to a higher false positive rate [6,7].
It has been shown that a negative D-dimer test can rule out an acute PE in 60 % of patients aged <40 years, but in only 5 % of patients above 80 years [4]. Consequently, older patients undergo unnecessary and abdicable further diagnostic investigations.
ADJUSTING D-DIMER CUT-OFF VALUES TO AGE
Very soon after implementation of the D-dimer test in clinical practice, raising its cut-off value has been claimed in order to improve specificity and thus, reduce the false positive rate of the D-dimer test in older age groups [8].
However, some authors worried that such an approach might inevitably increase the proportion of false negative results [9].
In 2010, Douma et al demonstrated for the first time both a statistically plausible and clinically practicable approach [10]. For their retrospective analysis, Douma et al adopted four cohorts of outpatients from three prospective multicenter studies (n= 5132 consecutive patients with clinically suspected pulmonary embolism).
The authors presented an age-adjusted D-dimer cut-off value which gradually increases with age: Age × 0.01 mg/L. By applying this simple adjusting formula to outpatients >50 years, the age-related adverse effects such as the false positive rate could considerably be reduced while hardly impairing the (clinically required) sensitivity.
The elegant approach of Douma et al was based upon dividing all patients >50 years in 10-year age groups (decades). Using receiver operating characteristic (ROC) curves, the optimal D-dimer cut-off value for each decade was derived by augmenting the specificity as much as possible without any loss in sensitivity.
A linear regression analysis of the cut-off values plotted against the age group led to the regression coefficient which represented the increase of the D-dimer cut-off value per decade. After dividing this coefficient by 10, an individual multiplication factor for each age could be obtained.
Since then, we and others confirmed this approach in elderly patients [11,12,13,14,15,16].
PERFORMANCE OF THE AGE ADJUSTED D-DIMER CUT-OFF VALUES
In a recent study, we analyzed a retrospective cohort of 1033 outpatients presenting to our emergency department with suspected acute PE/DVT [16].
We found that with the conventional cut-off value of <0.5 mg/L, the proportion of negative D-dimer results decreased from 73 % in patients from 50 to 59 years to 24 % in patients >80 years. Using the age-adjusted D-dimer cut-off value, this proportion only diminished from 76 % to 32 % in the corresponding age groups.
The relative increase of patients below the cut-off value is shown in Fig. 2a.
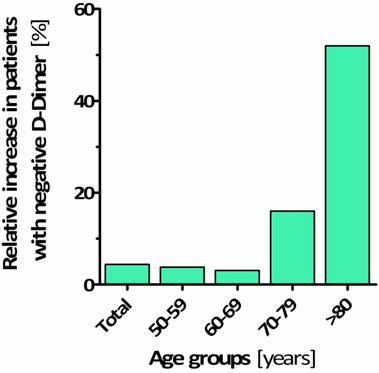
(a)
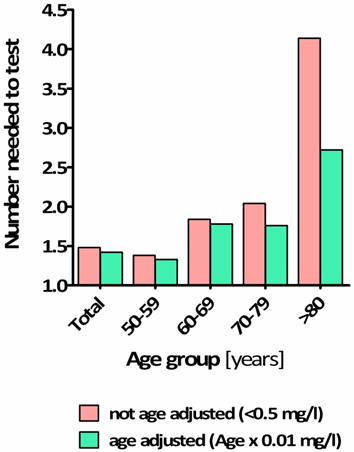
(b)
(c)
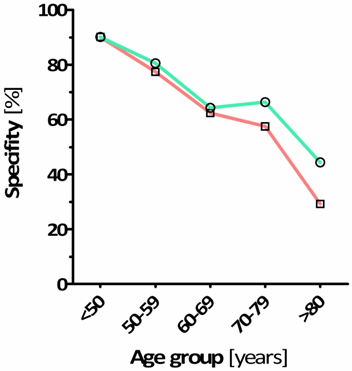
FIG. 2: Performance of age-adjusted D-dimer values in a retrospective cohort of 1033 outpatients presenting to our emergency department with suspected acute PE/DVT [16]. a) Relative increase of patients with a negative D-dimer test result by applying the age-adjusted cut-off values; b) Number needed to test (NNT) of the conventional and age-adjusted D-dimer cut-off values, presenting the number of D-dimer tests to rule out one PE/DVT; c) Increase in specificity by applying age-adjusted D-dimer cut-off values.
A more accessible depiction is the number needed to test (NNT), which presents the number of D-dimer tests to rule out one PE/DVT. Applying the conventional D-dimer cut-off value, the NNT increased from 1.4 in the age group 50-59 years to 4.1 in patients >80 years, while with the age-adjusted cut-off values, it merely increased from 1.3 to 2.7 in the corresponding age groups (Fig. 2b).
Without substantial loss in the sensitivity, specificity increased from 29 % in the age group >80 years using the conventional cut-off value to 44 % with the age-adjusted cut-off values (Fig. 2c).
Our mono-centric results are consistent with data from a recently published review and meta-analysis by Schouten et al who systematically analyzed 13 independent cohorts including 12,497 patients to evaluate the diagnostic accuracy of age-adjusted D-dimer cut-off values in older patients [17].
Beyond simple validation, the authors generated a hypothetical cohort of 5000 patients >50 years, in which – based on the pooled data of the reviewed studies – application of age adjustment resulted in a correct exclusion of venous thromboembolism in 453 extra patients (9 %) at the expense of only 10 new false negative test results (0.2 %).
Thus, the concern that adjusting the D-dimer cut-off values to the age would dramatically increase the false negative results could not be confirmed, at least in this retrospective dataset.
A noteworthy aspect is that in all studies validating the original age adjustment of Douma et al, five different D-dimer assays were used and a total of 15 cohorts tested [10].
However, according to the low error rate (proportion of missed PE/DVT of total number of negative D-dimer results) in all studies validating the new cut-off values remained <1 % (Verma et al [16]: 0.8 %; Douma et al [10]: 0.2 to 0.6 % depending on the cohort; Douma et al [11]: 0.8 % combined for all cohorts; Penaloza et al [13]: 0.8 % combined for all cohorts; Schouten et al [14]: 1.0 %.), the choice of the D-dimer assay seems to be of minor importance.
Moreover, the approach of age-adjusting D-dimer cut-off values has only been validated in outpatients with suspected PE/DVT. In hospitalized patients, D-dimer levels might not only be increased in case of PE/DVT, but also in context of malignant diseases, severe systemic inflammation, pregnancy or after surgery [18].
It is thus unlikely that age adjustment would improve the performance of D-dimers in inpatients. In addition, it must be considered that the benefit from applying age-adjusted D-dimer cut-off values decreases with increasing PE/DVT prevalence settings [17], which is also the case in hospitalized patients.
COST EFFECTIVENESS OF THE NEW D-DIMER CUT-OFF VALUES
A recent cost analysis study showed that (unadjusted) D-dimer measurement in cases of suspected PE is highly cost-saving under the age of 80 years. Above 80 years, the cost-saving effect of D-dimer is diminished, but not completely abolished [19].
A preliminary cost analysis of our retrospective cohort of 1033 outpatients with suspected acute PE/DVT [16] indicated a hypothetical total savings of 6200 € only for avoiding imaging diagnostics in 31 patients >50 years (over a period of 3 years), if the age-adjusted cut-off values were applied (Fig. 3).
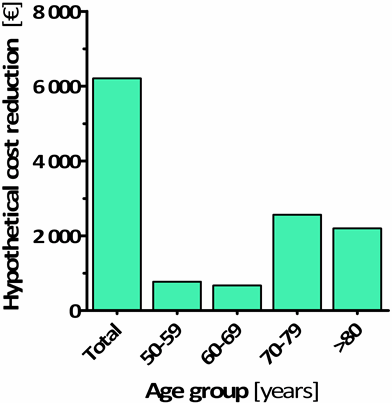
FIG. 3: Hypothetical cost reduction of avoidable CT imaging for each age group by applying the age-adjusted D-dimer cut-off values. Data shown for our preliminary in-house analysis on 1033 patients [16].
The cost-saving effect was already apparent in the age group >70 years.
However, the real potential for cost reduction can be assumed to be significantly higher, since the expenses for staff (transporting service, hospital care, logistics) and utilizing the hospital infrastructure (bed occupancy, CT availability) were not considered in this analysis.
CONCLUSION AND OUTLOOK
In conclusion, age adjustment of the D-dimer cut-off value increases the specificity for the exclusion of venous thromboembolism in higher age groups without overly affecting sensitivity. Thus, the proportion of elderly patients, in whom a thromboembolic event can be ruled out, increases.
The decrease of the false positive results leads to a reduction of unnecessary diagnostic investigations. Not only older patients would benefit from reducing redundant diagnostic imaging (e.g. radiation exposure, risks of contrast-media application), but also costs could be reduced.
We assume that in the medium term, age-adjusted D-dimer cut-off values will be established in the diagnostic strategy of an acute PE/DVT in the emergency department.
The current version of the interdisciplinary guideline “Diagnosis and therapy of DVT and PE” of the German Society of Angiology (2010) already refers to such an approach [20].
However, before implementing age-adjusted cut-off levels into daily clinical practice in the emergency department, a prospective study is required to confirm the clinical utility, cost effectiveness and ease of use in daily patient care.
KEY FACTS
- The concentration of the fibrin degradation product D-dimer increases with age. Thus, the D-dimer test to rule out thromboembolic events has a high false positive rate in elderly patients.
- Adjusting the D-dimer cut-off values to the age of outpatients >50 years increases specificity while hardly affecting sensitivity.
- By reducing the proportion of false-positive results, the age-adjusted D-dimer cut-off increases the proportion of older patients, in whom an acute thromboembolic event can be safely excluded.
- Age-adjusting D-dimer cut-off values might help save resources by reducing unnecessary diagnostic investigations and its complication.
- Before implementing in clinical daily practice, age-adjusted D-dimer cut-off values need to be tested in a prospective study.
Read more about d-dimer:
- Causes of increased D-dimer
- The clinical use of a D-dimer assay
- Comparing D-dimer assays using likelihood ratios and Fagan nomograms
- Assessment of plasma D-dimer as a diagnostic and prognostic aid for abdominal aortic aneurysm
- D-dimer assays - pitfalls of analytical comparisons
- The role of D-dimer in diagnosis of venous thromboembolism – a review
References+ View more
- Torbicki A., Perrier A., Konstantinides S., Agnelli G., Galie N., Pruszczyk P., Bengel F., et al.: Guidelines on the diagnosis and management of acute pulmonary embolism: the Task Force for the Diagnosis and Management of Acute Pulmonary Embolism of the European Society of Cardiology (ESC). Eur Heart J 2008; 29 (18): 2276-2315.
Perrier A., Roy P. M., Sanchez O., Le Gal G., Meyer G., Gourdier A. L., Furber A., et al.: Multidetector-row computed tomography in suspected pulmonary embolism. N Engl J Med 2005; 352 (17): 1760-1768.
van Belle A., Buller H. R., Huisman M. V., Huisman P. M., Kaasjager K., Kamphuisen P. W., Kramer M. H., et al.: Effectiveness of managing suspected pulmonary embolism using an algorithm combining clinical probability, D-dimer testing, and computed tomography. JAMA 2006; 295 (2): 172-179.
Righini M., Goehring C., Bounameaux H. and Perrier A.: Effects of age on the performance of common diagnostic tests for pulmonary embolism. Am J Med 2000; 109 (5): 357-361.
Der Sahakian G., Claessens Y. E., Allo J. C., Kansao J., Kierzek G. and Pourriat J. L.: Accuracy of D-Dimers to Rule Out Venous Thromboembolism Events across Age Categories. Emerg Med Int 2010; 2010 185453.
Tardy B., Tardy-Poncet B., Viallon A., Lafond P., Page Y., Venet C. and Bertrand J. C.: Evaluation of D-dimer ELISA test in elderly patients with suspected pulmonary embolism. Thromb Haemost 1998; 79 (1): 38-41.
Masotti L., Ceccarelli E., Cappelli R. and Forconi S.: Plasma D-dimer levels in elderly patients with suspected pulmonary embolism. Thromb Res 2000; 98 (6): 577-579.
Hager K. and Platt D.: Fibrin degeneration product concentrations (D-dimers) in the course of ageing. Gerontology 1995; 41 (3): 159-165.
Righini M., de Moerloose P., Reber G., Perrier A. and Bounameaux H.: Should the D-dimer cut-off value be increased in elderly patients suspected of pulmonary embolism? Thromb Haemost 2001; 85 (4): 744.
Douma R. A., le Gal G., Sohne M., Righini M., Kamphuisen P. W., Perrier A., Kruip M. J., et al.: Potential of an age adjusted D-dimer cut-off value to improve the exclusion of pulmonary embolism in older patients: a retrospective analysis of three large cohorts. BMJ 2010; 340 c1475.
Douma R. A., Tan M., Schutgens R., Bates S. M., Perrier A., Legnani C., Biesma D. H., et al.: Age-dependent D-dimer cut-off value increases the number of older patients in whom deep vein thrombosis can be safely excluded. Haematologica 2012;
Jaffrelot M., Le Ven F., Le Roux P. Y., Tissot V., Rame E., Salaun P. Y. and Le Gal G.: External validation of a D-dimer age-adjusted cut-off for the exclusion of pulmonary embolism. Thromb Haemost 2012; 107 (5): 1005-1007.
Penaloza A., Roy P. M., Kline J., Verschuren F., G L. E. G., Quentin-Georget S., Delvau N., et al.: Performance of age-adjusted D-dimer cut-off to rule out pulmonary embolism. J Thromb Haemost 2012; 10 (7): 1291-1296.
Schouten H. J., Koek H. L., Oudega R., Geersing G. J., Janssen K. J., van Delden J. J. and Moons K. G.: Validation of two age dependent D-dimer cut-off values for exclusion of deep vein thrombosis in suspected elderly patients in primary care: retrospective, cross sectional, diagnostic analysis. BMJ 2012; 344 e2985.
van Es J., Mos I., Douma R., Erkens P., Durian M., Nizet T., van Houten A., et al.: The combination of four different clinical decision rules and an age-adjusted D-dimer cut-off increases the number of patients in whom acute pulmonary embolism can safely be excluded. Thromb Haemost 2012; 107 (1): 167-171.
Verma N., Willeke P., Bicsan P., Lebiedz P., Pavenstadt H. and Kumpers P.: [Age-adjusted D-dimer cut-offs to diagnose thromboembolic events : Validation in an emergency department.]. Med Klin Intensivmed Notfmed 2013;
Schouten H. J., Geersing G. J., Koek H. L., Zuithoff N. P., Janssen K. J., Douma R. A., van Delden J. J., et al.: Diagnostic accuracy of conventional or age adjusted D-dimer cut-off values in older patients with suspected venous thromboembolism: systematic review and meta-analysis. BMJ 2013; 346 f2492.
Dempfle C. E.: Bestimmung des D-Dimer-Antigens in der klinischen Routine. Dtsch Arztebl 2005; 102 (7): 428-432.
Righini M., Nendaz M., Le Gal G., Bounameaux H. and Perrier A.: Influence of age on the cost-effectiveness of diagnostic strategies for suspected pulmonary embolism. J Thromb Haemost 2007; 5 (9): 1869-1877.
Angiologie D. G. f.: S2-Leitlinie: Diagnostik und Therapie der Venenthrombose und der Lungenembolie. 2010;
Wells P. S., Anderson D. R., Rodger M., Ginsberg J. S., Kearon C., Gent M., Turpie A. G., et al.: Derivation of a simple clinical model to categorize patients probability of pulmonary embolism: increasing the models utility with the SimpliRED D-dimer. Thromb Haemost 2000; 83 (3): 416-420.
References
- Torbicki A., Perrier A., Konstantinides S., Agnelli G., Galie N., Pruszczyk P., Bengel F., et al.: Guidelines on the diagnosis and management of acute pulmonary embolism: the Task Force for the Diagnosis and Management of Acute Pulmonary Embolism of the European Society of Cardiology (ESC). Eur Heart J 2008; 29 (18): 2276-2315.
Perrier A., Roy P. M., Sanchez O., Le Gal G., Meyer G., Gourdier A. L., Furber A., et al.: Multidetector-row computed tomography in suspected pulmonary embolism. N Engl J Med 2005; 352 (17): 1760-1768.
van Belle A., Buller H. R., Huisman M. V., Huisman P. M., Kaasjager K., Kamphuisen P. W., Kramer M. H., et al.: Effectiveness of managing suspected pulmonary embolism using an algorithm combining clinical probability, D-dimer testing, and computed tomography. JAMA 2006; 295 (2): 172-179.
Righini M., Goehring C., Bounameaux H. and Perrier A.: Effects of age on the performance of common diagnostic tests for pulmonary embolism. Am J Med 2000; 109 (5): 357-361.
Der Sahakian G., Claessens Y. E., Allo J. C., Kansao J., Kierzek G. and Pourriat J. L.: Accuracy of D-Dimers to Rule Out Venous Thromboembolism Events across Age Categories. Emerg Med Int 2010; 2010 185453.
Tardy B., Tardy-Poncet B., Viallon A., Lafond P., Page Y., Venet C. and Bertrand J. C.: Evaluation of D-dimer ELISA test in elderly patients with suspected pulmonary embolism. Thromb Haemost 1998; 79 (1): 38-41.
Masotti L., Ceccarelli E., Cappelli R. and Forconi S.: Plasma D-dimer levels in elderly patients with suspected pulmonary embolism. Thromb Res 2000; 98 (6): 577-579.
Hager K. and Platt D.: Fibrin degeneration product concentrations (D-dimers) in the course of ageing. Gerontology 1995; 41 (3): 159-165.
Righini M., de Moerloose P., Reber G., Perrier A. and Bounameaux H.: Should the D-dimer cut-off value be increased in elderly patients suspected of pulmonary embolism? Thromb Haemost 2001; 85 (4): 744.
Douma R. A., le Gal G., Sohne M., Righini M., Kamphuisen P. W., Perrier A., Kruip M. J., et al.: Potential of an age adjusted D-dimer cut-off value to improve the exclusion of pulmonary embolism in older patients: a retrospective analysis of three large cohorts. BMJ 2010; 340 c1475.
Douma R. A., Tan M., Schutgens R., Bates S. M., Perrier A., Legnani C., Biesma D. H., et al.: Age-dependent D-dimer cut-off value increases the number of older patients in whom deep vein thrombosis can be safely excluded. Haematologica 2012;
Jaffrelot M., Le Ven F., Le Roux P. Y., Tissot V., Rame E., Salaun P. Y. and Le Gal G.: External validation of a D-dimer age-adjusted cut-off for the exclusion of pulmonary embolism. Thromb Haemost 2012; 107 (5): 1005-1007.
Penaloza A., Roy P. M., Kline J., Verschuren F., G L. E. G., Quentin-Georget S., Delvau N., et al.: Performance of age-adjusted D-dimer cut-off to rule out pulmonary embolism. J Thromb Haemost 2012; 10 (7): 1291-1296.
Schouten H. J., Koek H. L., Oudega R., Geersing G. J., Janssen K. J., van Delden J. J. and Moons K. G.: Validation of two age dependent D-dimer cut-off values for exclusion of deep vein thrombosis in suspected elderly patients in primary care: retrospective, cross sectional, diagnostic analysis. BMJ 2012; 344 e2985.
van Es J., Mos I., Douma R., Erkens P., Durian M., Nizet T., van Houten A., et al.: The combination of four different clinical decision rules and an age-adjusted D-dimer cut-off increases the number of patients in whom acute pulmonary embolism can safely be excluded. Thromb Haemost 2012; 107 (1): 167-171.
Verma N., Willeke P., Bicsan P., Lebiedz P., Pavenstadt H. and Kumpers P.: [Age-adjusted D-dimer cut-offs to diagnose thromboembolic events : Validation in an emergency department.]. Med Klin Intensivmed Notfmed 2013;
Schouten H. J., Geersing G. J., Koek H. L., Zuithoff N. P., Janssen K. J., Douma R. A., van Delden J. J., et al.: Diagnostic accuracy of conventional or age adjusted D-dimer cut-off values in older patients with suspected venous thromboembolism: systematic review and meta-analysis. BMJ 2013; 346 f2492.
Dempfle C. E.: Bestimmung des D-Dimer-Antigens in der klinischen Routine. Dtsch Arztebl 2005; 102 (7): 428-432.
Righini M., Nendaz M., Le Gal G., Bounameaux H. and Perrier A.: Influence of age on the cost-effectiveness of diagnostic strategies for suspected pulmonary embolism. J Thromb Haemost 2007; 5 (9): 1869-1877.
Angiologie D. G. f.: S2-Leitlinie: Diagnostik und Therapie der Venenthrombose und der Lungenembolie. 2010;
Wells P. S., Anderson D. R., Rodger M., Ginsberg J. S., Kearon C., Gent M., Turpie A. G., et al.: Derivation of a simple clinical model to categorize patients probability of pulmonary embolism: increasing the models utility with the SimpliRED D-dimer. Thromb Haemost 2000; 83 (3): 416-420.
May contain information that is not supported by performance and intended use claims of Radiometer's products. See also Legal info.
Register for the related webinar
The Benefit of Using a D-dimer Assay with a High Clinical Specificity
Presented by Karin Strandberg, MD, PhD, Assoc. Prof.
Join the webinarAcute care testing handbook
Get the acute care testing handbook
Your practical guide to critical parameters in acute care testing.
Download nowScientific webinars
Check out the list of webinars
Radiometer and acutecaretesting.org present free educational webinars on topics surrounding acute care testing presented by international experts.
Go to webinars