Printed from acutecaretesting.org
October 2011
Choosing cut-offs for NT-proBNP
BACKGROUND
Heart failure (HF) is a complex syndrome and many definitions of this syndrome have been presented. In recent years, most definitions have emphasized the need for both the presence of symptoms of HF and physical signs of fluid retention [1].
The use of plasma concentrations of natriuretic peptides such as B-type natriuretic peptide (BNP) and N-terminal pro-B-type natriuretic peptide (NT-proBNP) as an aid in diagnosing and staging HF, making hospitalization/discharge decisions, and identifying patients at risk for clinical events is evidence based.
The choice of cut-off determines the clinical performance of any biochemical test. Often the upper limit of the reference interval is used to distinguish healthy from sick. Furthermore all test results have to be interpreted in the specific clinical context.
The reference range for NT-proBNP varies depending on the nature of the control population. The NT-proBNP values are related to, for example, age and body mass index (BMI). It should be noted that only few data are available on healthy subjects in whom cardiac dysfunction was ruled out by echocardiography [2].
The choice of NT-proBNP cut-off depends on the anticipated use of the test. In several trials of patients with acute symptoms, the optimal NT-proBNP cut-off for diagnosis of acute HF has been found to be considerably higher than the optimal cut-offs observed in studies of outpatient populations. Furthermore the cut-offs differ for rule-in and rule-out.
The population is ageing. This means that the prevalence of heart failure will increase as the prevalence of the disease is increasing with age. Therefore it is relevant to decide whether or not to use age-dependent reference intervals for clinical biochemistry parameters.
GUIDELINES
Official guidelines are available for the use of natriuretic peptides. Examples are the ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2008 [1] and the NACB Biomarkers of acute coronary syndromes and heart failure 2007 [3].
The ESC guidelines give specific cut-off values in the recommendations.
FIG. 1: Flowhart for the diagnosis of heart failure (HF) using NT-proBNP in untreated patients with symptoms suggestive of HF (extract from ESC guidelines)
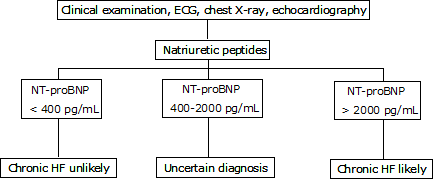
The NACB guidelines do not mention specific cut-offs in the recommendations. However, in the text they quote various studies and their results. Furthermore a table showing clinical performance (sensitivity, specificity, predictive values and accuracy) is presented.
TABLE I: Predictive values at specific cut-offs (Extract from NACB guidelines)
| Cut-off, pg/mL |
300 |
450 |
600 | 900 | 1000 |
| Positive predictive value |
62 % |
68 % |
73 % |
86 % |
78 % |
| Negative predictive value | 99 % |
99 % |
97 % |
94 % |
91 % |
When the NACB performance characteristics are compared to the values used in the ESC recommendations, it can be seen that at 400 pg/mL the negative predictive value is 99 %; thus at this cut-off it is very unlikely that the test will misclassify a sick person.
It also shows that at values below 1000 pg/mL the positive predictive values are not high enough to conclude a final diagnosis based on the NT-proBNP results.
AGE-ADJUSTED CUT-OFFS
When NT-proBNP is used as a clinical tool for diagnosis of acute decompensated HF, age-adjusted cut-offs are often applied and this has been shown in several studies to be appropriate. The PRIDE study [4] is a frequently quoted reference.
The use of age-adjusted cut-offs can be discussed. Some may assume that with age it is acceptable that a certain amount of deterioration may exist and that it is only when it becomes extreme that the healthcare system deems the treatment appropriate. Others find the age-adjusted cut-offs useful in clinical practice.
Age may not be independently associated with increased levels of NT-proBNP.
However, a number of abnormalities, more frequently observed in older patients, seem to be significantly associated with the risk of increased levels of NT-proBNP.
We are becoming increasingly aware of inter-organ cross-talk and thus the total estimation of the biological condition of an individual patient, accompanying disorders, and classification according to the year of birth is important for the diagnosis and interpretation of laboratory results.
What calls for using age-related cut-offs is that in addition to cardiovascular variables that influence the concentrations of natriuretic peptides, old age (and renal dysfunction) may also lead to higher values in the absence of heart failure.
Examples of age-related cut-offs have been given by Januzzi et al (2006) [5]. They found that for ruling-out acute heart failure, a single age-independent cut-off (300 pg/mL) was superior. However, for ruling-in they found that it was optimal to use age-stratified cut-offs. The cut-offs are presented in Table II.
TABLE II: Age-stratified cut-offs for diagnosis of acute heart failure
|
Age |
Cut-off |
Sensitivity, % |
|
< 50 years |
< 450 pg/mL |
97 |
|
50-75 years |
< 900 pg/mL |
90 |
|
> 75 years |
< 1800 pg/mL |
85 |
Some find that the PRIDE study guidelines should only be applied until the presence or absence of comorbidities in the patient is diagnosed [6].
Bernstein et al (2011) [6] has re-evaluated the reference range for interpreting an NT-proBNP elevation under the assumption that the interpretation based on the PRIDE study results [4] is not solely dependent on age and that it does not account sufficiently for concomitant morbidities, which can increase the NT-proBNP levels independent of heart failure.
Bernstein et al found the following with respect to NT-proBNP and age:
- Sharp increase in NT-proBNP for persons > 50 years
- Increase in NT-proBNP at 7 % per decade for persons > 50 years
- Decrease in estimated glomerular filtration rate (eGFR) at 4 % per decade for persons > 50 years
- Slope of NT-proBNP increase with age is related to proportion of patients with eGFR < 90
- NT-proBNP increase can be delayed or accelerated based on disease comorbidities
The final conclusion of Bernstein et al is that NT-proBNP levels can be accurately assessed only after removal of the major confounding comorbidities that increase NT-proBNP.
They suggest that clinicians may apply the PRIDE criteria initially, but should consider adopting an alternative approach. Bernstein et al established a new range after determining the absence of comorbidities.
They found that for normal persons over 50 years of age and with no comorbidities, the upper limit of the reference range is ~1000 pg/mL.
“STANDARDIZATION” OF NT-proBNP ASSAYS
All commercial NT-proBNP assays are either produced under a license from a specific company or by that company itself.
To get a license from that company the new NT-proBNP method has to correlate very strictly to the company’s method.
So even though there is no official international standardization of NT-proBNP there is a certain “harmonization”’ of all the marketed diagnostic NT-proBNP assays.
This also means that the results of all NT-proBNP assays can be used interchangeably. Therefore no matter which NT-proBNP assay you use, you can use the cut-off data from any study that you find is comparable to your own setting.
References+ View more
- The Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2008 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association of the ESC (HFA) and endorsed by the European Society of Intensive Care Medicine (ESICM): ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2008. Eur Heart J 2008; 29: 2388–2442.
- Januzzi JL, Richards AM, eds. An International Consensus Statement Regarding Amino Terminal Pro-B-Type Natriuretic Peptide Testing: The International NT-proBNP Consensus Panel. Am J Cardiol. 2008; 101(3A).
- Christenson RH, ed. The National Academy of Clinical Biochemistry. Laboratory Medicine Practice Guidelines. Biomarkers of Acute Coronary Syndromes and Heart Failure. 2007.
- Januzzi JL, Camargo CA, Anwaruddin S et al. The N-terminal Pro-BNP investigation of dyspnea in the emergency department (PRIDE) study. Am J Cardiol 2005; 95(8): 948-54.
- Januzzi JL, van Kimmenade R, Lainchbury J et al. NT-proBNP testing for diagnosis and short-term prognosis in acute destabilized heart failure: an international pooled analysis of 1256 patients. Eur Heart J 2006; 27: 330-37.
- Bernstein LH, Zions MY, Alam ME et al. What is the best approximation of reference normal for NT-proBNP? Clinical levels for enhanced assessment of NT-proBNP (CLEAN). JMLD 2011; 2(2): 16-21
References
- The Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2008 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association of the ESC (HFA) and endorsed by the European Society of Intensive Care Medicine (ESICM): ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2008. Eur Heart J 2008; 29: 2388–2442.
- Januzzi JL, Richards AM, eds. An International Consensus Statement Regarding Amino Terminal Pro-B-Type Natriuretic Peptide Testing: The International NT-proBNP Consensus Panel. Am J Cardiol. 2008; 101(3A).
- Christenson RH, ed. The National Academy of Clinical Biochemistry. Laboratory Medicine Practice Guidelines. Biomarkers of Acute Coronary Syndromes and Heart Failure. 2007.
- Januzzi JL, Camargo CA, Anwaruddin S et al. The N-terminal Pro-BNP investigation of dyspnea in the emergency department (PRIDE) study. Am J Cardiol 2005; 95(8): 948-54.
- Januzzi JL, van Kimmenade R, Lainchbury J et al. NT-proBNP testing for diagnosis and short-term prognosis in acute destabilized heart failure: an international pooled analysis of 1256 patients. Eur Heart J 2006; 27: 330-37.
- Bernstein LH, Zions MY, Alam ME et al. What is the best approximation of reference normal for NT-proBNP? Clinical levels for enhanced assessment of NT-proBNP (CLEAN). JMLD 2011; 2(2): 16-21
Acute care testing handbook
Get the acute care testing handbook
Your practical guide to critical parameters in acute care testing.
Download nowScientific webinars
Check out the list of webinars
Radiometer and acutecaretesting.org present free educational webinars on topics surrounding acute care testing presented by international experts.
Go to webinars









