Printed from acutecaretesting.org
June 2009
D-dimer as a rule-out test for deep venous thrombosis: Gold standards and bias in negative predictive value
BACKGROUND
Venous thromboembolism is a disorder that most commonly has two manifestations, thrombosis in the deep veins of the leg (deep venous thrombosis (DVT)) and pulmonary embolism.The measurement of D-dimer, degradation products of circulating cross-linked fibrin formed during the activation of the coagulation system, is frequently used in clinical practice as a rule-out test for venous thromboembolism.
A good rule-out test is one that, if negative, makes the likelihood of the disease in question sufficiently low that a clinician may exclude it from consideration in the care of the patient.
In the usual approach to diagnostic-testing research, the results of the test being evaluated are compared to the results of a “gold standard” (or “reference standard”) test in an appropriate group of patients suspected of having the disease in question.
The data are then arranged in a two-by-two table (TABLE 1) that allows the indices of test efficacy to be calculated. For a rule-out test, the key issue is that the frequency of patients with DVT having a negative test (“false negative tests”) must be very low.
If this is so, the indices of interest for ruling out disease, sensitivity and negative predictive value (defined in TABLE 1) will be high.
TABLE 1: The two-by-two table for diagnostic testing research
TP = true positive tests; FP = false positive tests; FN = false negative tests; TN = true negative tests; NPV = negative predictive value
| Test |
|
|||||
| Positive | TP | FP | ||||
| Negative | FN | TN | ||||
Sensitivity |
= |
TP |
| ____________ | ||
| TP + FN |
NPV |
= |
TN |
| ____________ | ||
| FN + TN |
The gold standard test should be an accepted way of determining “the truth” regarding diagnosis. Typical examples of gold standard tests are biopsy results for cancer, coronary arteriography for coronary artery disease and hemoglobin electrophoresis for sickle cell disease.
In the past 25 years, more than 40 studies have been published comparing D-dimer levels with a gold standard for lower-extremity DVT [1,2]. Until 1995, D-dimer studies usually selected lower-extremity venography as the gold standard for DVT diagnosis [1].
In more recent years, paralleling clinical practice, duplex ultrasonography has assumed a more prominent role as the gold standard. Since March 1995, duplex ultrasound alone was used as the gold standard in nine studies [3].
Despite the fact that clinicians now use duplex ultrasound as the test of choice for the evaluation of patients with suspected lower-extremity DVT [4], it has disadvantages as a gold standard for lower-extremity DVT research.
This is because duplex ultrasound, although it is very accurate in detecting thrombosis in thigh veins, has limited ability to image DVT in the smaller calf veins [5]. In clinical practice, this limitation has been circumvented by a strategy of repeating the ultrasound on subsequent days in order to detect extension of calf DVT to the thigh veins [4].
However, in D-dimer research, the use of a single ultrasound as the gold standard creates the potential for bias. This potential for bias is demonstrated in TABLE 2. A gold standard that images both thigh and calf DVT, such as venography, will enable all patients with lower-extremity DVT to be properly counted as diseased (TABLE 2 A).
On the other hand, to the extent that a gold standard such as duplex ultrasound fails to fully image the calf veins, diseased patients are counted in the non-diseased category (TABLE 2 B).
This results in biased indices of test efficacy. For example, because the true sensitivity of a D-dimer test for thigh DVT is higher than the sensitivity for calf DVT, the measured sensitivity appears higher than it actually is.
Most importantly for a rule-out test, the negative predictive value appears to be higher than it actually is because false negative calf DVT tests are counted erroneously as true negatives in the calculation of negative predictive value (TABLE 2).
TABLE 2: Effect of different gold standards on content of two-by-two table cells
TP = true positive tests; FP = false positive tests; FN = false negative tests; TN = true negative tests; NPV = negative predictive value
A. Results with gold standard that images both thigh and calf veins
| D-dimer test |
|
|||||
| Positive | TPThigh + TPCalf | FP | ||||
| Negative | FNThigh + FNCalf | TN | ||||
NPVThigh and calf |
= |
TN |
| ______________________ | ||
| All negative D-dimer tests |
B. Results with gold standard that images thigh veins only
| D-dimer test |
|
|||||
| Positive | TPThigh | TPCalf + FP | ||||
| Negative | FNThigh | FNCalf + TN | ||||
NPVThigh |
= |
FNCalf + TN |
| ______________________ | ||
| All negative D-dimer tests |
EFFECT OF THE CHOICE OF GOLD STANDARD ON NEGATIVE PREDICTIVE VALUE
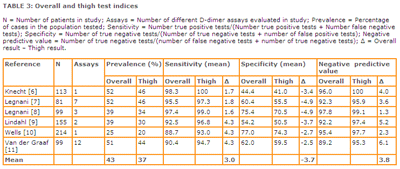
The presence and magnitude of this bias have been demonstrated [3] and are summarized in TABLE 3. Six studies [6-11] were identified that utilized venography to verify the presence or absence of thigh and calf DVT in all subjects.TABLE 3: Overall and thigh test indices
click to enlarge
DISCUSSION
D-dimer is an easily performed blood test that has advantages over other diagnostic tests for lower-extremity DVT. The alternatives, venography and ultrasonography, are radiologic imaging tests that require the availability of someone with the skills to perform and interpret the tests.
In addition, venography carries the risks of radiologic contrast (allergic reactions and renal damage) and also of causing a DVT. Because D-dimer assays are positive in a variety of common conditions including some with signs and symptoms of DVT (e.g. surgery on hip or knee, trauma, cellulitis or malignancy), they are not appropriate for use as rule-in tests where a low false positive rate is needed.
On the other hand, while studies of D-dimer as a rule-out test have shown promise, care must be taken in interpreting results of the studies that have used ultrasound as the gold standard.
To the extent that ultrasound misses isolated calf DVT, the important test index of negative predictive value will appear to be higher than its true value. The potential magnitude of this bias is large enough to be of clinical significance.
It is possible in ultrasound studies that the actual magnitude of this bias is less than reported here, since ultrasonographers often extend their evaluation to the trifurcation of the popliteal vein, or even more distal, and report the presence of calf DVT when found.
In evaluating D-dimer studies using ultrasound as the gold standard, careful reading of the ultrasound methods will provide the necessary information to determine how well the calf veins have been evaluated.
It is also possible that the true differences are even larger than shown here. Venous thromboembolism frequently is not limited to the deep veins of the legs. Silent pulmonary embolism occurs in 40-50 % of patients with thigh DVT [12].
It is thus possible that there are additional patients with undetected pulmonary emboli counted in the non-diseased column along with the patients with undetected calf DVT.
Venous thromboembolism diagnostic-testing research presents particular challenges because the best gold standards, venography of the legs and pulmonary angiography, are invasive, expensive and potentially risky.
In addition, unlike radiologic imaging tests, the D-dimer test has the important advantage of potentially being used to rule out venous thromboembolism in all locations including calf, thigh, pelvis, upper extremity and lungs.
However, to establish this role for D-dimer, researchers must choose carefully the appropriate gold standard, one that is comprehensive and not prone to underdiagnosis. This would be one that includes complete testing for both DVT (e.g. venography) and pulmonary embolism (e.g. spiral computed tomography or pulmonary arteriography) [2].
Because of cost and risk, studies of this design are difficult to carry out. An alternative approach is the use of management studies, where patients are evaluated using diagnostic algorithms with outcome assessment to determine safety and cost-effectiveness.
Most management trials have combined a probability assessment of DVT with D-dimer results, with the results determining whether further testing would be performed [13,14].
References+ View more
- Becker DM, Philbrick JT, Bachuber TL, Humphries JE. D-dimer testing and acute venous thromboembolism. Arch Intern Med. 1996; 156: 939-46.
- Heim SW SJ, Siadaty MS, Philbrick JT. D-dimer testing for deep venous thrombosis: a metaanalysis. Clin Chem. 2004; 50(7): 1136-47.
- Philbrick JT, Heim S. The D-dimer test for deep venous thrombosis: gold standards and bias in negative predictive value. Clin Chem.
- Ginsberg JS. Management of venous thromboembolism. New England Journal of Medicine. 1996; 335: 1816-28.
- Becker DM, Philbrick JT, Abbitt PL. Real-time ultrasonography for the diagnosis of lower extremity deep venous thrombosis: the wave of the future? Arch Intern Med. 1989; 149: 1731-34.
- Knecht MF, Heinrich F. Clinical evaluation of an immunoturbidimetric D-dimer assay in the diagnostic procedure of deep vein thrombosis and pulmonary embolism. Thrombosis Research. 1997; 88: 413-17.
- Legnani C, Pancani C, Palareti G, et al. Comparison of new rapid methods for D-dimer measurement to exclude deep vein thrombosis in symptomatic outpatients. Blood Coagulation and Fibrinolysis. 1997; 8: 296-302.
- Legnani C, Pancani C, Palareti G, Guazzaloca G, Coccheri S. Contribution of a new, rapid, quantitative and automated method for D-dimer measurement to exclude deep vein thrombosis in symptomatic outpatients. Blood Coagulation and Fibrinolysis. 1999; 10: 69-74.
- Lindahl TL, Lundahl TH, Ranby M, Fransson SG. Clinical evaluation of a diagnostic strategy for deep venous thrombosis with exclusion by low plasma levels of fibrin degradation product D-dimer. Scandinavian Journal of Clinical Laboratory Investigation. 1998; 58: 307-16.
- Wells PS, Brill-Edwards P, Stevens P, et al. A novel and rapid whole-blood assay for D-Dimer in patients with clinically suspected deep vein thrombosis.Circulation. 1995; 91: 2184-87.
- van der Graaf F, van den Borne H, van der Kolk M, de Wild PJ, Janssen GWT, van Uum SHM. Exclusion of deep venous thrombosis with D-dimer testing.Thrombosis and Haemostasis. 2000; 83: 191-98.
- Meignan MRJ, Gauthier H, Brunengo F, Claudel S, Sagnard L, et al. Systemic lung scans reveal a high frequency of silent pulmonary embolism in patients with proximal deep venous thrombosis. Arch Intern Med. 2000; 160: 159-64.
- Kearon C, Ginsberg JS, Douketis J, et al. Management of suspected deep venous thrombosis in outpatients by using clinical assessment and D-dimer testing.Annals of Internal Medicine. 2001; 135: 108-11.
- Wells PS AD, Rodger M, Fogie M, Kearon C, Dreyer J, et al. Evaluation of D-dimer in the diagnosis of suspected deep-vein thrombosis. New England Journal of Medicine. 2003; 349: 1227-35.
References
- Becker DM, Philbrick JT, Bachuber TL, Humphries JE. D-dimer testing and acute venous thromboembolism. Arch Intern Med. 1996; 156: 939-46.
- Heim SW SJ, Siadaty MS, Philbrick JT. D-dimer testing for deep venous thrombosis: a metaanalysis. Clin Chem. 2004; 50(7): 1136-47.
- Philbrick JT, Heim S. The D-dimer test for deep venous thrombosis: gold standards and bias in negative predictive value. Clin Chem.
- Ginsberg JS. Management of venous thromboembolism. New England Journal of Medicine. 1996; 335: 1816-28.
- Becker DM, Philbrick JT, Abbitt PL. Real-time ultrasonography for the diagnosis of lower extremity deep venous thrombosis: the wave of the future? Arch Intern Med. 1989; 149: 1731-34.
- Knecht MF, Heinrich F. Clinical evaluation of an immunoturbidimetric D-dimer assay in the diagnostic procedure of deep vein thrombosis and pulmonary embolism. Thrombosis Research. 1997; 88: 413-17.
- Legnani C, Pancani C, Palareti G, et al. Comparison of new rapid methods for D-dimer measurement to exclude deep vein thrombosis in symptomatic outpatients. Blood Coagulation and Fibrinolysis. 1997; 8: 296-302.
- Legnani C, Pancani C, Palareti G, Guazzaloca G, Coccheri S. Contribution of a new, rapid, quantitative and automated method for D-dimer measurement to exclude deep vein thrombosis in symptomatic outpatients. Blood Coagulation and Fibrinolysis. 1999; 10: 69-74.
- Lindahl TL, Lundahl TH, Ranby M, Fransson SG. Clinical evaluation of a diagnostic strategy for deep venous thrombosis with exclusion by low plasma levels of fibrin degradation product D-dimer. Scandinavian Journal of Clinical Laboratory Investigation. 1998; 58: 307-16.
- Wells PS, Brill-Edwards P, Stevens P, et al. A novel and rapid whole-blood assay for D-Dimer in patients with clinically suspected deep vein thrombosis.Circulation. 1995; 91: 2184-87.
- van der Graaf F, van den Borne H, van der Kolk M, de Wild PJ, Janssen GWT, van Uum SHM. Exclusion of deep venous thrombosis with D-dimer testing.Thrombosis and Haemostasis. 2000; 83: 191-98.
- Meignan MRJ, Gauthier H, Brunengo F, Claudel S, Sagnard L, et al. Systemic lung scans reveal a high frequency of silent pulmonary embolism in patients with proximal deep venous thrombosis. Arch Intern Med. 2000; 160: 159-64.
- Kearon C, Ginsberg JS, Douketis J, et al. Management of suspected deep venous thrombosis in outpatients by using clinical assessment and D-dimer testing.Annals of Internal Medicine. 2001; 135: 108-11.
- Wells PS AD, Rodger M, Fogie M, Kearon C, Dreyer J, et al. Evaluation of D-dimer in the diagnosis of suspected deep-vein thrombosis. New England Journal of Medicine. 2003; 349: 1227-35.
May contain information that is not supported by performance and intended use claims of Radiometer's products. See also Legal info.
Acute care testing handbook
Get the acute care testing handbook
Your practical guide to critical parameters in acute care testing.
Download nowScientific webinars
Check out the list of webinars
Radiometer and acutecaretesting.org present free educational webinars on topics surrounding acute care testing presented by international experts.
Go to webinars








