Printed from acutecaretesting.org
June 2005
Reducing sharps injury risk in intensive care
Healthcare workers in intensive care and critical care units (ICUs/CCUs) face unique challenges, and some unique risks, when it comes to sharps safety.
Like emergency departments (EDs), ICUs are often fast-paced; crises and codes requiring high-intensity therapies and rapid interventions are common in this environment.
Critically ill patients require more procedures, tests and blood draws performed on a daily basis than patients in other settings—and these, in turn, require the use of more sharps.
In addition, some invasive and diagnostic procedures are performed in ICUs that are not typically performed in other patient units, such as bronchoscopies and thoracenteses.
Data from the Centers for Disease Control and Prevention on healthcare workers (HCWs) with occupationally acquired HIV/AIDS confirm that workers in ICUs are at higher risk of bloodborne pathogen transmission.
A 1997 analysis revealed that, out of 46 HCWs infected with HIV from percutaneous injuries, 11 (24 %) were exposed in ICUs—the location with the highest number of cases (followed by patient rooms, with 10 cases) [1].
In one well-documented case, a nurse working in an ICU was stuck by an IV catheter used on a patient with end-stage AIDS; she was infected with HIV as a result [2].
The SIROH group in Italy (Italian Study Group on Occupational HIV Infection Risk) examined five years of sharps injury and mucocutaneous exposure data (1994-1998) from 18 hospitals, and developed percutaneous exposure rates by job category and work area [3].
For nurses in intensive care units, the exposure rate was 7.1 per 100 full-time equivalents (FTEs), and for physicians, 4.1 per 100 FTEs. The mucocutaneous exposure rate in ICUs was 3.7 per 100 FTEs for nurses, and 2.3 for physicians.
METHODS
To understand more about sharps injury risks in ICUs, we analyzed five years of EPINet data (1998-2002) [4] from the EPINet Multi-Hospital Needlestick and Blood Exposure database.
EPINet (Exposure Prevention Information Network) is a standardized surveillance system for tracking percutaneous injuries and blood exposures in healthcare settings.
Developed by the International Health Care Worker Safety Center at the University of Virginia in 1992, it is now used by more than 1,500 healthcare facilities in the US; customized versions have been developed for use in Canada, the UK, Ireland, Australia, Germany, Sweden, Spain, Italy, Japan and many other countries around the world.
EPINet consists of a Uniform Needlestick and Sharp Object Injury Report form and a Uniform Blood and Body Fluid Exposure Report form, with software programmed in Microsoft® Access for entering, analyzing and reporting exposure data.
Since 1993, the Center has collected data on an annual basis from an aggregate total of more than 80 healthcare facilities that use the EPINet system and voluntarily participate in the EPINet research network.
With ten years of data, it is the longest-standing database in the US of healthcare workers’ at-risk exposures to blood and body fluids.
Exposures can be analyzed based on job category, location in which the exposure occurred, device causing injury, mechanism of exposure, and a variety of other characteristics.
To extract data on percutaneous injuries (PIs) in ICUs, we selected “intensive/critical care unit” under the category “where injury occurred” (16 different healthcare settings are listed).
During the five-year period selected, 82 facilities contributed data to the EPINet network; of these, 21 were teaching hospitals and 61 were non-teaching hospitals.
RESULTS
A total of 10,441 percutaneous injuries (PIs) were
reported to the EPINet network from 1998 to 2002; of those, 7 %
(687) occurred in ICUs/CCUs—the fourth-ranking location after
patient rooms (31 %), ORs (29 %) and EDs (9 %).
FIGURE 1 shows the job categories of workers reporting injuries in ICUs/CCUs: nurses sustained 61 % of injuries (for all other hospital settings, the fraction for nurses was 41 %); physicians, 16 % (interns/residents/fellows, 12 %; attendings, 4 %); respiratory therapists, 8 %; and phlebotomists and housekeepers, 3.5 % each.
Of injuries to nurses, 41 % (171/418) involved blood-filled, hollow-bore needles and thus were high risk for bloodborne pathogen transmission. (Of high-risk injuries to nurses, the largest proportion, 20 %, occurred while drawing venous blood).
For interns/residents, the proportion of injuries from blood-filled needles was much lower—26 %. However, for respiratory therapists, who perform a high percentage of arterial blood draws in intensive care settings, 73 % of injuries were from blood-filled, hollow-bore needles.
FIGURE 1:
JOB CATEGORIES OF WORKERS IN INTENSIVE/CRITICAL CARE UNITS
REPORTING PERCUTANEOUS INJURIES
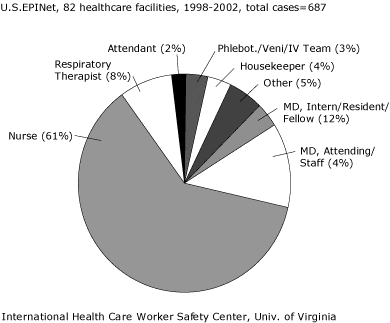
FIGURE 2 shows devices causing injuries in ICUs/CCUs. The largest proportion of injuries were caused by disposable syringes (33 %). Almost a third of disposable syringe injuries involved drawing venous or arterial blood.
Butterfly needles accounted for 11 % of injuries; IV catheters, 9 %; suture needles, 9 %; blood gas syringes, 5 %; and prefilled syringes, unattached hypodermic needles and scalpels, 3 % each. Overall, 42 % of PIs in ICUs involved blood-filled needles; for all other settings, that fraction was much lower—25 %.
FIGURE 2:
DEVICES CAUSING PERCUTANEOUS INJURIES IN INTENSIVE/CRITICAL CARE
UNITS
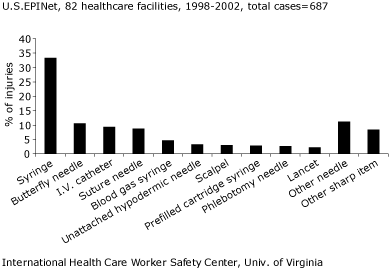
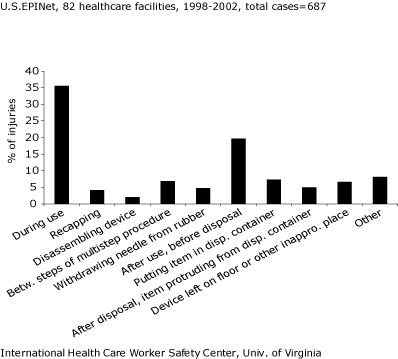
FIGURE 3 shows when injuries in ICUs occurred in the use/disposal cycle. Thirty-six percent of injuries occurred during use of the device; 20 % occurred after use but before disposal; 7 % occurred while putting a device into a disposal container, and an additional 7 % from a device left on the floor, table, bed or other inappropriate place.
Many, if not most, of the injuries that occur after use of a device are preventable by using a safety-engineered device that covers the needle or sharp after use.
FIGURE 3:
PERCUTANEOUS INJURIES IN INTENSIVE/CRITICAL CARE UNITS: WHEN
INJURIES ORCCURED
DISCUSSION
To help reduce injury risk, the appropriate
safety-engineered equipment should be used for drawing venous and
arterial blood. Syringes should not be used for venous blood
drawing; instead, phlebotomy or butterfly needles (with a
protective feature) should be used, because they allow blood to be
drawn directly into a blood tube [5].
If a syringe must be used, the sample should not be transferred to a blood tube by inserting the needle into the tube’s rubber stopper; this increases needlestick risk, because the worker can miss the stopper and stick his or her hand instead, or sustain a rebound stick when pulling the needle out of the stopper.
A safety needle that can be separated from the syringe barrel should be used instead; once the sample is drawn, the safety feature is activated and the protected needle removed from the syringe.
A blood transfer device is then attached to the syringe and the blood tube inserted into the transfer device.
For arterial blood draws, safety syringes that are specifically designed for performing arterial blood gases (ABGs) should be used. Staff in ICUs should have an opportunity to evaluate different brands of safety ABG syringes, and should be comfortable and proficient with the one they choose.
Once the safety feature on the ABG syringe has been activated, the sample should be placed in a biohazard bag with a zipper closing, and transported quickly to the lab to preserve its integrity.
Safety ABG syringes and kits are available from several companies [6].
Almost half of the injuries from ABG syringes (48 %) occurred during use of the device—a higher proportion than any other hollow-bore needle device in ICUs (for butterfly needles, 39 % occurred during use; for IV catheters, 27 %).
Needle insertions at the radial artery site—the preferred site for ABGs—can be painful for patients and cause them to move suddenly or jerk their arms, and the caregiver to be stuck as a result.
A review of 111 case descriptions (EPINet, 2000-2002) of needlestick injuries that occurred while drawing arterial blood revealed that 29 % (32/111) were caused by patient movement. Use of a local anesthetic can help minimize patient movement and thus reduce needlestick risk [7].
Butterfly needles are the second leading cause of injury in ICUs. With tubing attached, these devices can be awkward to handle and difficult to get into a sharps container; 14 % of injuries from butterfly needles occurred during disposal.
In addition to using safety butterfly needles, staff in ICUs should ensure that sharps containers have openings large enough to accommodate this bulky device, and that containers are replaced before becoming overfilled.
The proportion of injuries in ICUs from suture needles has risen significantly over the 10 years that EPINet data have been collected: in 1993, they accounted for 3 % of injuries; in 1998, 7 %; in 2002, 12 %. By way of comparison, suture needles account for about 2 % of injuries in patient rooms.
One possible explanation is that safer alternatives to sharp-tipped suture needles have not been as widely adopted in US hospitals as other types of safety-engineered needles.
Blunt-tip suture needles, which are sharp enough for suturing subcutaneous tissue but not sharp enough, in most cases, to penetrate skin, provide a safer alternative to sharp-tip ones [8-9].
Since 81 % of suture needle injuries in ICUs occurred during use of the device, utilizing alternatives to suturing, such as tissue adhesives, adhesive strips, staples and adhesive catheter securement devices should significantly decrease injury risk.
CRITICAL CARE: SAFETY PRECAUTIONS
The following recommendations can help decrease the
risk of needlestick injury to healthcare workers in intensive care
settings. In the US, use of safety-engineered devices and safer
work practices are required under the Needlestick Safety and
Prevention Act (2000) and the revised bloodborne pathogens standard
(2001), enforced by the Occupational Safety and Health
Administration (OSHA).
- Use safety-engineered phlebotomy and butterfly needles for drawing venous blood, not syringes
- Use safety-engineered ABG syringes for arterial blood draws; for radial ABGs, use a local anesthetic to minimize patient movement and reduce needlestick risk
- Make sure sharps containers have openings wide enough to accommodate butterfly needles with attached tubing, and make sure containers are replaced before becoming overfilled
- Utilize blunt-tip suture needles when possible for suturing subcutaneous tissue, and alternatives to suturing, such as tissue adhesives, surgical staples and adhesive catheter securement devices for skin closure
Implementing these recommendations will help ensure the safest possible environment for healthcare workers in ICUs, and, in the US, will also help ensure compliance with OSHA’s requirement to eliminate or minimize employees’ exposure to bloodborne pathogens.
References+ View more
- Centers for Disease Control and Prevention. Location of percutaneous exposure in 46 health care workers with documented occupationally acquired HIV; United States through June 1997. Advances in Exposure Prevention. 1998;3(3):33.
- Arnold L. A nurse with a mission. Advances in Exposure Prevention. 1996;2(2):1,9-11.
- Puro V, De Carli G, Petrosillo N, Ippolito G. Risk of exposure to bloodborne infection for Italian healthcare workers, by job category and work area. Studio Italiano Rischio Occupazionale da HIV Group. Infection Control and Hospital Epidemiology. 2001;22(4):206-10.
- International Health Care Worker Safety Center, University of Virginia Health System. EPINet Multihospital Needlestick and Sharp-Object Injury Data Report, Intensive Care/Critical Care Units, 1998-2002 (687 injuries, 82 hospitals contributing data).
- Jagger J, Perry J. Risky phlebotomy with a syringe. Nursing. 2001;31(2):73.
- ECRI. Arterial blood gas syringes. (Chapter 4, Evaluations). Sharps Safety & Needlestick Prevention (2nd edition). Plymouth Meeting, PA: ECRI, 2003; pp. 47-51.
- Levitan RM. Reducing pain during arterial blood drawing—minimizing patient movement. Advances in Exposure Prevention. 1995;2(1):5.
- Centers for Disease Control and Prevention. Evaluation of blunt suture needles in preventing percutaneous injuries among health-care workers during gynecologic surgical procedures - New York City, March 1993-June 1994. MMWR. 1997;46:25-29.
- Jagger J, Bentley M, Tereskerz P. A study of patterns and prevention of blood exposures in OR personnel. AORN Journal. 1998;67(5):979-96.
References
- Centers for Disease Control and Prevention. Location of percutaneous exposure in 46 health care workers with documented occupationally acquired HIV; United States through June 1997. Advances in Exposure Prevention. 1998;3(3):33.
- Arnold L. A nurse with a mission. Advances in Exposure Prevention. 1996;2(2):1,9-11.
- Puro V, De Carli G, Petrosillo N, Ippolito G. Risk of exposure to bloodborne infection for Italian healthcare workers, by job category and work area. Studio Italiano Rischio Occupazionale da HIV Group. Infection Control and Hospital Epidemiology. 2001;22(4):206-10.
- International Health Care Worker Safety Center, University of Virginia Health System. EPINet Multihospital Needlestick and Sharp-Object Injury Data Report, Intensive Care/Critical Care Units, 1998-2002 (687 injuries, 82 hospitals contributing data).
- Jagger J, Perry J. Risky phlebotomy with a syringe. Nursing. 2001;31(2):73.
- ECRI. Arterial blood gas syringes. (Chapter 4, Evaluations). Sharps Safety & Needlestick Prevention (2nd edition). Plymouth Meeting, PA: ECRI, 2003; pp. 47-51.
- Levitan RM. Reducing pain during arterial blood drawing—minimizing patient movement. Advances in Exposure Prevention. 1995;2(1):5.
- Centers for Disease Control and Prevention. Evaluation of blunt suture needles in preventing percutaneous injuries among health-care workers during gynecologic surgical procedures - New York City, March 1993-June 1994. MMWR. 1997;46:25-29.
- Jagger J, Bentley M, Tereskerz P. A study of patterns and prevention of blood exposures in OR personnel. AORN Journal. 1998;67(5):979-96.
May contain information that is not supported by performance and intended use claims of Radiometer's products. See also Legal info.
Acute care testing handbook
Get the acute care testing handbook
Your practical guide to critical parameters in acute care testing.
Download nowRelated webinar
Evolution of blood gas testing Part 1
Presented by Ellis Jacobs, PhD, Assoc. Professor of Pathology, NYU School of Medicine.
Watch the webinar









